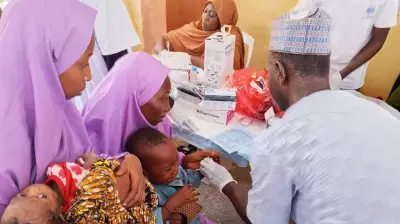
Beyond the Delivery Room: How SARMAAN Bridges Maternal Care and Child Survival in Nigeria
Maternal health and child survival in Nigeria are intricately connected, with programs like SARMAAN employing integrated care strategies to significantly reduce under-five mortality and enhance overall health outcomes. The nation cannot address child survival effectively without a thorough examination of maternal health, as healthy pregnancies and safe deliveries are merely the starting points in a critical continuum of care.
The Critical Link Between Maternal and Child Health
Recent national statistics reveal that approximately 110 out of every 1,000 Nigerian children die before reaching age five, equating to roughly one in nine children. This alarming under-five mortality rate is among the highest globally, paralleled by a maternal mortality ratio that also ranks among the world's worst. These figures underscore a fragile continuum where women and children are lost, highlighting the necessity of treating maternal and child health as interconnected issues rather than separate problems.
Dr. Zeenaht Abdullahi, an obstetrician and gynaecologist, emphasizes this linkage: "In my experience, maternal health outcomes and the survival of children in their early years are interwoven, where one significantly influences the other. Healthy mothers during pregnancy and postpartum can provide essential care, such as exclusive breastfeeding, infection prevention through cord care, and early detection of developmental anomalies. Their physical and mental well-being enables them to prevent, detect, and seek timely care for their children."
Challenges in Post-Delivery Care
Despite efforts to ensure safe deliveries, the healthcare system often disengages once a birth is recorded, leaving families to navigate communities with varying levels of support. Some mothers return to areas with accessible immunisation schedules, clean water, and prompt treatment for illnesses, while others face distant clinics, overstretched health workers, frequent stock-outs, and threats from preventable diseases like diarrhoea, pneumonia, and malaria. This disparity means that while both scenarios might be counted as maternal health successes, only one child may survive months later, a reality rarely captured in official statistics.
Solutions and the Role of Integrated Care
Global and national analyses consistently identify simple, preventive interventions that could avert the majority of under-five deaths if reliably delivered. These include exclusive breastfeeding, full immunisation, vitamin A supplementation, insecticide-treated bed nets, good nutrition, and prompt treatment of common illnesses. Scaling up these proven strategies in high-mortality settings like Nigeria could prevent hundreds of thousands of deaths annually. However, success hinges on supporting mothers to access services, trust the health system, and engage repeatedly during their children's first five years.
Viewing maternal health and child survival as a single continuum clarifies the task: antenatal care, safe delivery, post-natal visits, immunisation, nutrition counselling, and community-based prevention should be integrated investments rather than competing programs. Each contact point, from pregnancy check-ups to home visits by community health workers, can be leveraged to layer additional life-saving interventions, avoiding the common pattern of intense effort around childbirth followed by neglect.
SARMAAN: A Model for Integration
Initiatives like SARMAAN exemplify this integrated approach by working through mothers in high-risk communities to expand access to azithromycin mass drug administration for children aged one to 59 months. Based on evidence from West African trials, biannual azithromycin distribution has been associated with reduced all-cause mortality in young children. While not a magic bullet and requiring careful use to mitigate antimicrobial resistance, it offers a practical tool to combat infections that claim many young lives.
SARMAAN's significance lies in its centering of mothers, utilizing existing trust and contact points from antenatal clinics, deliveries, and post-natal visits. Mothers treated with dignity and trust in the healthcare system are more likely to accept azithromycin for their toddlers, complete immunisations, and seek early care for danger signs. This approach integrates child survival interventions with maternal health efforts, rather than operating in isolation.
Policy Implications and Future Directions
The program also contributes to policy discussions by generating local data on coverage, safety, community acceptance, and feasibility, providing Nigerian decision-makers with evidence on how azithromycin administration can complement routine child health services and primary healthcare strengthening. It offers a model for layering targeted, evidence-based tools onto existing maternal and newborn care platforms, avoiding the need for new vertical projects.
Nigeria has committed to ambitious global targets on maternal and child mortality, but current rates indicate a long road ahead. To change this narrative, the country must extend care beyond the delivery room, viewing child protection as part of the same commitment that begins in pregnancy. This requires financing and staffing primary health centres, supporting frontline workers, and designing programs that recognize mothers as partners. Initiatives like SARMAAN demonstrate the potential to transform statistics into action by empowering mothers, bridging the gap between delivery and early childhood, and treating child survival as a natural extension of maternal health.