Jehovah's Witnesses' Blood Transfusion Ban Poses Severe Health Risks in Nigeria
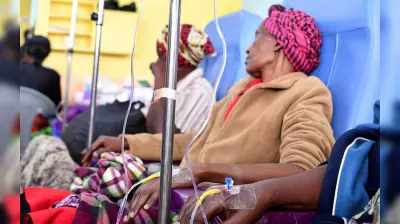
Jehovah's Witnesses' unwavering stance against blood transfusions continues to generate significant health concerns across Nigeria, where adherence to this doctrine has contributed to preventable fatalities. Under the religious group's teachings, accepting a blood transfusion is considered a grave sin, strictly forbidden even in life-threatening medical emergencies. This report delves into the tragic outcomes for individuals who refused transfusions and examines the broader challenges within Nigeria's healthcare system in addressing such cases.
Case Studies Highlighting Fatal Consequences
In August 2025, a somber gathering in Ota, Ogun State, mourned the death of Tutu, a 16-year-old Jehovah's Witness diagnosed with systemic lupus erythematosus (SLE). Despite receiving care at Lagos State University Teaching Hospital (LASUTH), her parents refused a necessary blood transfusion, citing religious convictions. They signed multiple refusal forms and discharged her, believing divine intervention would suffice. Tutu passed away days later, underscoring how religious prohibitions can exacerbate health crises.
Similarly, Aunty Esther, a popular internet personality from Lagos, faced a dire situation after being diagnosed with advanced breast cancer. Despite public donations exceeding N30 million for her treatment, she declined chemotherapy due to her Jehovah's Witness beliefs, as it required a blood transfusion to manage anaemia. Her death shortly afterward sparked widespread debate on the intersection of faith and medical necessity.
Medical and Legal Perspectives on the Issue
Dr. Michael Olusina Ajidahun, a digital health strategist, emphasized that Nigeria's healthcare system is ill-equipped to handle cases where patients refuse critical treatments for religious reasons. He noted that while bloodless surgeries exist, they are often impractical in emergencies or without advanced equipment. The country's ongoing health crises, including outbreaks of diseases like Lassa fever, further strain resources, making transfusions a vital, life-saving option in many scenarios.
Legal precedents, such as the Supreme Court case involving infant Tega Esabunor, have addressed conflicts between medical treatment and religious beliefs. In that instance, court-ordered transfusion saved the child's life, highlighting the ethical dilemmas faced by healthcare providers. Journalist David Hundeyin, a former Jehovah's Witness, recounted his own childhood experience with a "death warrant" document prohibiting transfusions, criticizing the group's policies as cult-like and dangerous.
Why Jehovah's Witnesses Reject Blood Transfusions
Jehovah's Witnesses base their prohibition on biblical interpretations, citing scriptures like Genesis 9:4 and Acts 15:28-29 that command abstinence from blood. They view blood as sacred, representing life, and reject whole blood and its components—red cells, white cells, platelets, and plasma. Members risk being "disfellowshipped" for accepting transfusions, with teachings suggesting it could jeopardize their chance at eternal life in a paradise earth. Efforts to contact the Jehovah's Witnesses leadership in Nigeria for comment on potential policy revisions went unanswered.
Challenges in Implementing Bloodless Surgery in Nigeria
Bloodless surgery, advocated by Jehovah's Witnesses, involves techniques to minimize blood loss without transfusions, but its adoption in Nigeria faces significant hurdles. Dr. AbdulRasaq Ebiti of the Federal Medical Centre Ebute Metta explained that such procedures require expensive equipment and specialized training, often unavailable in public healthcare settings. Most Nigerian surgeons are trained to rely on transfusions as a backup, and infrastructural limitations hinder the widespread use of advanced, transfusion-free methods.
Dr. Adeniyi Ajibade, a transfusion medicine specialist, added that current realities in Nigeria make blood transfusions the standard practice, especially for conditions like sickle cell anemia. He noted that while Western countries have better resources for bloodless management, Nigeria's healthcare system prioritizes transfusions to save lives. Inquiries to the Ministry of Health regarding efforts to promote bloodless medicine received no response, reflecting broader systemic neglect.
These cases illustrate a critical tension between religious freedom and public health in Nigeria, where preventable deaths continue to rise due to doctrinal restrictions. As the country grapples with high mortality rates from treatable diseases, the need for balanced approaches that respect beliefs while ensuring medical safety remains urgent.